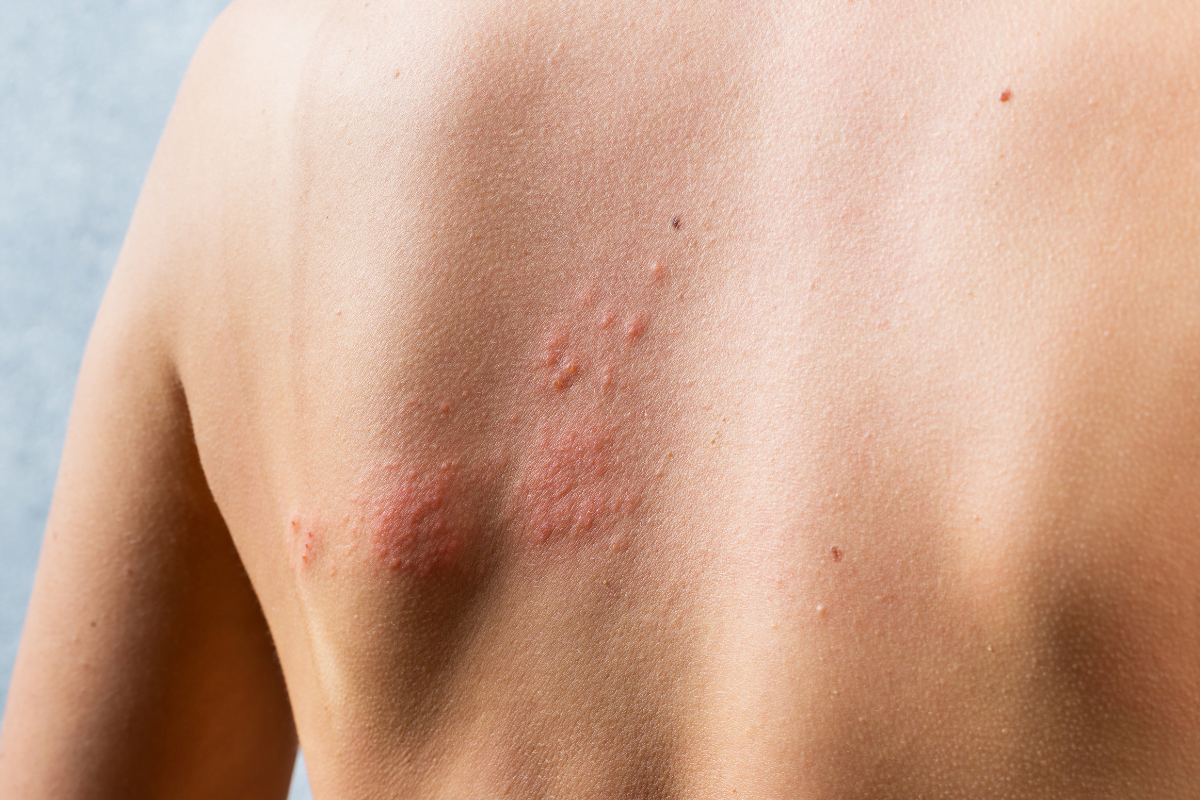
Porphyria cutanea tarda treatment usually centers on lowering excess porphyrins, reducing iron burden when it is part of the problem, and removing triggers that keep the disease active. For many people, that means therapeutic phlebotomy or a carefully supervised low-dose antimalarial, along with sun protection and a workup for factors such as alcohol use, estrogen exposure, hepatitis C, smoking, iron overload, and liver disease. This matters because PCT can keep causing fragile skin, blisters, scarring, and pigment changes on sun-exposed skin if the cause is not addressed.
Key Takeaways
- PCT is often manageable and may reach remission with the right plan.
- Main treatment paths are therapeutic phlebotomy and low-dose hydroxychloroquine or chloroquine.
- Iron studies, liver health, triggers, and anemia risk help shape treatment choice.
- Sun protection and gentle skin care are part of treatment, not extras.
- Follow-up matters because recurrence can happen even after improvement.
What PCT Is and Why Treatment Works
Porphyria cutanea tarda, often shortened to PCT, is the most common porphyria that mainly affects the skin. It happens when uroporphyrinogen decarboxylase, an enzyme involved in heme production, is not working well enough. Porphyrins then build up, mostly in the liver, and make the skin unusually sensitive to sunlight.
People often notice fragile skin on the hands, blistering after sun exposure, slow-healing erosions, crusting, milia, darker or lighter patches of skin, or increased facial hair. PCT often appears in adulthood, even when a person also has a genetic tendency in the background. The visible skin findings are real, but the process driving them is biochemical and often tied to iron and liver factors.
Because these symptoms overlap with other blistering disorders, treatment should follow proper testing rather than guesswork. Diagnosis often involves urine or plasma porphyrin studies, iron tests such as ferritin, and a review of liver-related risks. If you are still comparing skin conditions more broadly, the Dermatology Hub can help with orientation, while the Dermatology Product Hub is better for browsing medication categories.
PCT is often very manageable because the core problem can quiet down when the main drivers are treated. Treatment works by lowering the porphyrin load, lowering excess iron when it is contributing, and removing the triggers that keep the cycle going. That is also why common rash treatments, including steroids used for other skin problems, do not correct the underlying issue in PCT.
Why it matters: Skin healing usually follows after porphyrin levels start to fall.
How Porphyria Cutanea Tarda Treatment Is Chosen
The best porphyria cutanea tarda treatment depends on the full picture, not a single symptom or lab value. Clinicians usually look at confirmed porphyrin testing, ferritin and other iron studies, hemoglobin, liver status, alcohol and estrogen exposure, smoking, viral hepatitis risk, and whether repeat blood removal is practical and safe.
That review helps clarify the main management paths. If excess iron appears to be part of the problem and blood counts allow it, therapeutic phlebotomy is often considered. If phlebotomy is not a good fit, some patients may be considered for carefully supervised low-dose hydroxychloroquine or chloroquine. Medication review matters here because liver issues, other drugs, and individual tolerance can change the plan.
Before starting treatment, the care team may also look at how active the blistering is, whether the diagnosis is newly confirmed or recurrent, and whether there are other reasons to avoid blood removal or use extra caution with medication. Even practical details such as transportation, venous access, work schedule, and the ability to return for repeat labs can shape what is sustainable.
A durable plan is the one that is medically appropriate and realistic to follow. That may sound simple, but it is one reason PCT management is more personal than a one-size-fits-all checklist.
| Approach | When it may be considered | Main aim | What is monitored |
|---|---|---|---|
| Therapeutic phlebotomy | When iron overload appears contributory and blood counts support blood removal | Lower iron stores that can drive porphyrin buildup | Hemoglobin, ferritin, symptoms, and skin response |
| Low-dose hydroxychloroquine or chloroquine | When phlebotomy is not ideal or a medication approach fits better | Help mobilize excess porphyrins so the body can clear them | Liver status, other medicines, tolerance, and response |
| Trigger control and sun protection | For nearly everyone with PCT | Reduce ongoing skin injury and lower the chance of reactivation | Alcohol or estrogen exposure, smoking, liver issues, and healing |
The Two Main Treatment Paths
The established treatment paths are not competing trends. They are two different ways to lower the biochemical burden that drives the skin findings. One removes blood to reduce iron stores. The other uses a low-dose antimalarial medicine to help clear porphyrins.
Therapeutic phlebotomy
Therapeutic phlebotomy is planned blood removal done for medical reasons. In PCT, the goal is to bring down iron stores because excess iron can worsen the enzyme block behind the condition. Ferritin is often followed over time because it gives a useful signal about iron burden, though the target and pace are individualized.
Improvement is usually gradual rather than immediate. New blistering may settle before older skin changes fully fade. This is also not exactly the same as routine blood donation, even if the process looks similar from the outside. The schedule is shaped by labs, symptoms, and tolerance, not by a fixed public donation pattern.
Phlebotomy is not right for everyone. Anemia risk, poor venous access, frailty, and other health issues can change the balance. Some people also find repeated in-person visits hard to sustain. That is why the decision belongs in a clinician-guided plan rather than a generic online rule.
Low-dose antimalarial medicines
Hydroxychloroquine and chloroquine are older antimalarial drugs, but in PCT they may be used for a different reason. At carefully selected low doses, they can help move excess porphyrins out of the liver so they can be cleared. Because that effect can be strong, PCT regimens are typically more cautious than the way these medicines are used for some other conditions.
This option may be considered when repeated phlebotomy is hard to tolerate or not practical. It also needs thoughtful review. Liver disease, other medications, and individual risk factors can all matter. In some cases, the medication route may look simpler on paper but still require careful follow-up and lab monitoring.
If hydroxychloroquine is part of the conversation, neutral product pages such as Plaquenil and HCQS 200mg can show the kind of medicine involved, but they do not replace clinician guidance on fit, monitoring, or dosing.
BorderFreeHealth works with licensed Canadian partner pharmacies.
Whichever path is used, the goal is the same: stop new blistering, let the skin recover, and reduce the risk that active disease keeps damaging the skin and liver. Some people respond well to one strategy after another has been ruled out. Others need the plan adjusted over time as labs, tolerance, and trigger control change.
Trigger Control, Skin Care, and Liver Health
Even effective porphyria cutanea tarda treatment can stall if the main triggers stay active. Alcohol use, estrogen exposure, smoking, excess iron, hepatitis C, and other liver stressors are common themes in PCT care. Some people also have inherited tendencies that affect iron handling. That is why management is broader than a skin cream or a single prescription.
Sun protection matters from day one. PCT skin is fragile, and sunlight can worsen blistering on exposed areas such as the backs of the hands and forearms. Protective clothing, shade, and careful daily skin protection can reduce fresh damage while the underlying disease is being treated. This is often where people start to feel more in control.
Skin care in PCT is practical, not cosmetic. Lightweight sleeves or gloves for driving and outdoor chores may help protect fragile areas. Gentle cleansing, non-adhesive dressings when needed, and avoiding friction or picking can lower the chance of scarring and infection while healing is underway.
Because porphyrin buildup is closely tied to the liver, many treatment plans include liver-focused follow-up. That may involve reviewing alcohol use, checking liver tests, considering hepatitis evaluation when relevant, and discussing whether iron supplements or hormone exposures need a closer look. These are not side issues. They are part of the main treatment logic.
PCT is also a reminder that blistering skin problems are not all treated the same way. If you are sorting through a new dermatology diagnosis, neutral explainers such as Dupixent Explained, Cosentyx Uses, Otezla Uses, Apremilast Mechanism, and Humira Generic show how different treatment frameworks can be across skin conditions.
Quick tip: Photograph new blisters before they heal so follow-up visits have a clearer baseline.
What Follow-Up, Remission, and Recurrence Look Like
Most people want to know when treatment is working. The honest answer is that progress is often stepwise. Lab changes may improve before the skin fully catches up. Follow-up commonly focuses on blistering frequency, skin fragility, ferritin or other iron measures, porphyrin trends, liver tests, and whether the main triggers have been brought under control.
Many patients can reach remission, meaning new blistering settles and porphyrin levels come down. PCT is often one of the more manageable porphyrias because the disease process can quiet down when its drivers are addressed. Even so, older pigment changes, milia, or scarring may improve more slowly than the active disease itself.
Recurrence is still possible. PCT can reactivate if iron burden rises again or if triggers such as alcohol, estrogen exposure, smoking, or liver disease return to the forefront. That does not always mean treatment failed. It often means the underlying drivers need to be reviewed again.
If you are preparing for a visit about management of porphyria cutanea tarda, these questions often help:
- Which labs are being tracked and why
- Whether iron overload is part of your picture
- Which triggers matter most in your case
- How treatment response will be measured
- What symptoms should prompt earlier review
When required, prescriber details are checked before a pharmacy dispenses medication.
Practical issues count too. People without insurance may focus on cash-pay options, transportation for repeat visits, and whether clinic-based phlebotomy or medicine-based management is easier to sustain. Those concerns are valid. They do not replace medical decision-making, but they do shape what follow-up looks like in real life.
Good porphyria cutanea tarda treatment does not end when a blister dries up. It includes confirming the diagnosis, tracking the labs that match the cause, protecting the skin while healing happens, and reducing the drivers that could bring the condition back.
Authoritative Sources
- For a liver-focused overview, see the NIDDK page on porphyria.
- For genetic background and plain-language context, read the MedlinePlus Genetics entry on porphyria cutanea tarda.
- For a recent clinical review, see the PubMed summary on clinical management of porphyria cutanea tarda.
Further reading can help you prepare better questions for your care team. In practice, porphyria cutanea tarda treatment is usually a mix of trigger control, skin protection, and a clinician-guided plan to reduce iron burden or clear excess porphyrins over time.
This content is for informational purposes only and is not a substitute for professional medical advice.