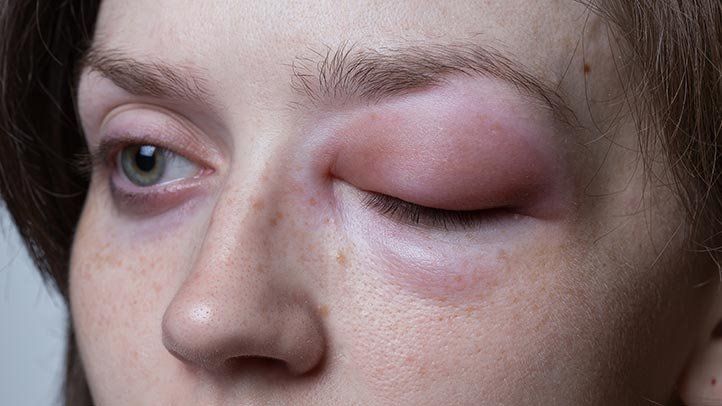
If you searched ‘What Is Angioedema: Symptoms, Triggers, and Treatment Guide,’ the short answer is this: angioedema is sudden swelling in deeper layers of the skin or lining tissues. It often affects the lips, eyelids, tongue, hands, feet, or genitals. It can appear with hives or happen on its own. Why this matters is simple: the cause changes the best response, and swelling in the tongue or throat can become dangerous fast.
Most episodes are acute, meaning short-lived, but some people have recurrent swelling over time. Because the pattern can point to allergy, medication effects, or inherited conditions, the first questions are usually what swelled, how fast it happened, whether hives were present, and whether breathing or swallowing changed.
Key Takeaways
- Angioedema is deep swelling, not just surface irritation.
- It may happen with hives, but not always.
- Common triggers include allergies, medications, infections, and inherited conditions.
- Throat swelling, breathing trouble, or faintness need emergency care.
- Treatment depends on the cause and whether histamine is involved.
What Angioedema Means Beneath The Skin
Angioedema is swelling caused by fluid leaking from small blood vessels into deeper tissue. Unlike a mild rash, it tends to feel puffy, firm, or tight. The skin may look normal, pink, or slightly red. The swelling often develops over minutes to hours and can take hours or a few days to settle, depending on the trigger.
Doctors often think about two broad pathways. The first is mast cell-mediated angioedema, meaning histamine and related allergy signals are driving the swelling. This form more often comes with hives, itching, flushing, or an obvious trigger such as a food, sting, or medication reaction. The second is bradykinin-mediated angioedema, which involves a different chemical pathway. It is more likely to cause swelling without hives and may be seen with certain blood pressure medicines, especially ACE inhibitors, or in hereditary angioedema.
Why The Cause Matters
The reason angioedema happens affects both risk and treatment. Histamine-driven episodes often respond to common allergy treatments. Bradykinin-driven swelling usually does not follow the same pattern. That is one reason recurrent lip or tongue swelling without hives deserves a careful history rather than guesswork.
For broader background on related conditions, the Allergy And Immunology hub can help you place angioedema in context.
BorderFreeHealth works with licensed Canadian partner pharmacies.
Symptoms And Warning Signs To Watch
The most common angioedema symptoms are sudden swelling of the lips, eyelids, face, tongue, hands, feet, or genitals. The area may feel stretched, warm, tender, or heavy rather than simply itchy. Some people notice tingling first. Others wake up with swelling that was not there the night before.
Angioedema can also affect mucous membranes, which are the moist linings inside the body. That means symptoms are not always visible on the skin. Swelling in the mouth or throat can change the voice, make swallowing hard, or create a tight sensation. Swelling in the gut can cause cramping, nausea, vomiting, or belly pain. These internal symptoms are easy to misread if you do not know angioedema can happen there too.
Why it matters: A swollen tongue or throat can block airflow even when the skin changes look limited.
Angioedema And Hives Are Related, But Not The Same
Hives and angioedema often overlap, but they affect different layers of tissue. Hives tend to sit closer to the skin surface and look like raised, itchy welts. Angioedema goes deeper and usually looks more like broad swelling than a cluster of bumps.
| Feature | Angioedema | Hives |
|---|---|---|
| Depth | Deeper tissue swelling | Surface skin welts |
| Common feel | Tight, sore, heavy, or warm | Very itchy |
| Common sites | Lips, eyelids, tongue, hands, feet | Anywhere on the skin |
| Appearance | Diffuse puffiness | Raised red or pale patches |
| May occur together | Yes | Yes |
This distinction matters because angioedema without hives can point toward medication effects, hereditary angioedema, or other non-allergic pathways rather than a simple allergic flare.
When Swelling Needs Urgent Care
Angioedema becomes an emergency when it affects breathing or raises concern for a severe allergic reaction. Trouble breathing, noisy breathing, sudden voice changes, swelling of the tongue, trouble swallowing saliva, fainting, chest tightness, or rapidly spreading swelling should be treated as urgent. Severe stomach pain with repeated vomiting can also deserve prompt evaluation, especially in people with recurrent unexplained episodes.
If symptoms start soon after a new medicine, food, sting, or another clear exposure, that timing is important to report. So is a family history of similar swelling. Even when a person has had angioedema before, a new throat symptom should not be treated as routine.
- Breathing changes — urgent evaluation
- Tongue or throat swelling — emergency risk
- Fainting or severe weakness — possible serious reaction
- Rapid spread — do not wait it out
- Severe belly pain — consider deeper swelling
Common Causes, Triggers, And Risk Factors
Angioedema causes fall into a few major groups. Allergic angioedema may follow foods, insect stings, latex, or medications. Non-allergic angioedema can be triggered by drugs, infections, physical pressure, or temperature changes. Some cases are hereditary, caused by an inherited problem in the C1 inhibitor system, which helps regulate swelling. Others are called idiopathic angioedema, meaning a clear cause is not found even after evaluation.
One especially important trigger is an ACE inhibitor, a common blood pressure medicine class. ACE inhibitor angioedema may happen without hives and can occur even after someone has taken the medication for a long time. That delayed pattern surprises many people. Other drugs can also cause or worsen swelling, which is why a full medication list matters.
Risk factors can include a personal or family history of swelling, a history of hives or allergies, certain medications, and prior unexplained episodes of face or lip swelling. In some people, stress, illness, dental work, or minor trauma seem to act more like triggers than root causes. The pattern over time often gives the strongest clues.
What Causes Angioedema Without Hives?
Angioedema without hives raises the chance of a non-histamine pattern. Medication effects, especially ACE inhibitors, hereditary angioedema, and some idiopathic cases are common reasons clinicians look more closely. That does not mean every case without hives is inherited or dangerous, but it does mean the workup may go beyond standard allergy questions.
Food concerns come up often, but there is no single universal list of foods to avoid with angioedema. If a specific food clearly triggered an episode, it makes sense to note that pattern and discuss it during evaluation. Without a clear link, broad food restriction can create confusion more than clarity.
When required, prescription details are checked with the prescriber before dispensing.
How Angioedema Is Diagnosed And Treated
Diagnosis starts with the story. Clinicians usually ask how fast the swelling appeared, whether hives or itching were present, what medicines or foods were involved, whether the belly or throat were affected, and whether relatives have had similar episodes. Photos from a phone can help, especially when the swelling has eased by the appointment.
Testing is not the same for everyone. A single, obvious allergic episode may need a different workup than recurrent swelling with no rash. In repeat or unexplained cases, especially when hereditary angioedema is a concern, clinicians may order blood tests related to complement proteins such as C4 and C1 inhibitor. The goal is not to test everything at once. It is to match the tests to the pattern.
Angioedema treatment also depends on the pattern. Histamine-related swelling may improve with antihistamines, corticosteroids, or emergency treatment for anaphylaxis when a severe allergic reaction is involved. Bradykinin-mediated angioedema usually needs a different approach, and specialist-directed therapies may be considered for hereditary angioedema or recurrent non-allergic swelling. If a medication appears to be the trigger, the prescriber may review whether an alternative is needed.
That is also why there is no single best antihistamine for every case. An antihistamine may help when histamine is driving the swelling, but it does not explain every episode. For recurrent or severe symptoms, the plan is usually built around the likely mechanism, the body areas involved, and how quickly symptoms escalate.
If a clinician is considering a histamine-blocking approach, some readers also look into options such as Histantil. The best fit still depends on the cause of swelling and the overall treatment plan.
Quick tip: Keep a simple log with timing, photos, new medicines, foods, infections, and stress around each episode.
If you are wondering whether swelling could be medication-related, a page like Synthroid Side Effects shows the kind of timing details clinicians use when reviewing possible reactions.
Living With Recurrent Or Unclear Swelling
Repeated angioedema can be frustrating because the episodes may look dramatic but still be hard to explain. A useful next step is often pattern recognition rather than panic. The goal is to understand whether the swelling behaves like allergy, medication-related swelling, hereditary angioedema, or an idiopathic pattern that needs ongoing follow-up.
These questions can make an appointment more productive:
- Timing — how fast it appeared
- Location — lips, face, throat, or gut
- Skin findings — hives, itching, or none
- Triggers — foods, stings, infections, pressure, medicines
- Family history — similar swelling in relatives
- Response pattern — what seemed to help or did not
That last point is especially useful. Swelling that repeatedly ignores typical allergy treatment may need a different explanation. The same is true for episodes linked to abdominal pain, family history, or ACE inhibitor use. Recurrent angioedema is often managed best with a plan that names likely triggers, lists emergency warning signs, and clarifies when specialist evaluation is worth considering.
Angioedema prevention is usually practical, not perfect. It may include avoiding confirmed triggers, reviewing medication lists after a reaction, keeping photos and notes from past episodes, and making sure family history is not overlooked. There is no one-size-fits-all prevention plan because angioedema is a pattern, not a single cause.
Some cross-border prescription options are cash-pay and depend on eligibility and jurisdiction.
Authoritative Sources
- A clear condition summary from Cleveland Clinic on angioedema
- A patient-friendly overview from Mayo Clinic on hives and angioedema
- Emergency-focused guidance from the NHS guide to angioedema
Further reading can help, but the key point is simple: angioedema is not one thing. The swelling pattern, the trigger, and the presence or absence of hives are what make the condition easier to understand.
This content is for informational purposes only and is not a substitute for professional medical advice.