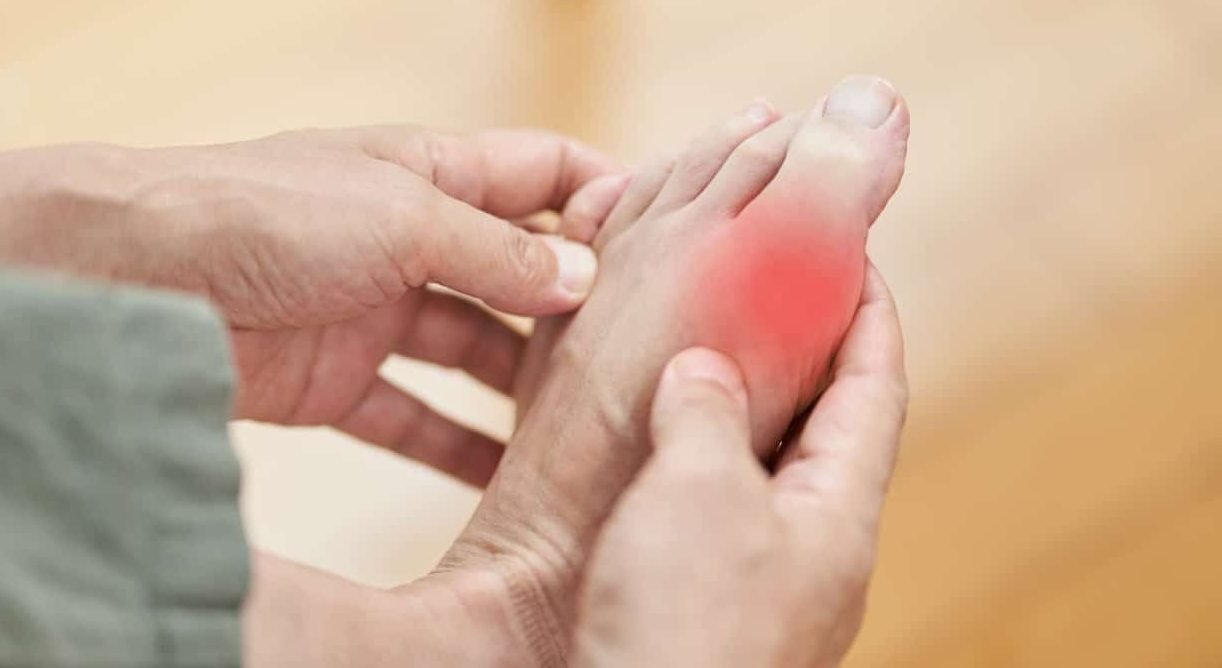
If you are asking what is hyperuricemia, the plain answer is this: it means your blood has more uric acid than your body can comfortably handle. Uric acid forms when the body breaks down purines, natural chemicals in your cells and in some foods. A high uric acid level may cause no symptoms, yet it can raise the chance of gout, uric acid kidney stones, or kidney strain in some people. Safer control starts with finding why the level is high, then matching diet, lifestyle, testing, and treatment decisions to your real risk.
Key Takeaways
- Hyperuricemia means serum uric acid is higher than expected on a blood test.
- Many people feel well, especially before gout or kidney stones appear.
- Common contributors include kidney function, genetics, alcohol, sugary drinks, certain foods, weight changes, and some medicines.
- Diet can help, but it is not the whole plan for everyone.
- Seek medical review for severe joint pain, fever, blood in urine, or intense side or back pain.
What is hyperuricemia in plain terms?
Hyperuricemia is a lab finding, not a symptom by itself. It means your serum uric acid level is above the range your lab or clinician considers typical. Many references describe elevated levels as above about 6 mg/dL for women and above about 7 mg/dL for men, but lab ranges vary. Your clinician should interpret the result with your age, sex, kidney function, medicines, and symptoms.
Uric acid is not automatically harmful. Your body makes it every day as part of normal cell turnover. The kidneys remove most of it through urine, while a smaller amount leaves through the gut. Problems can develop when the body makes too much, removes too little, or both.
When uric acid stays high, it may form sharp crystals. These crystals can settle in joints and trigger gout, a painful inflammatory arthritis. They can also contribute to uric acid kidney stones. Some people have asymptomatic hyperuricemia, meaning the blood level is high but they have no gout attacks, stones, or obvious symptoms.
Why it matters: A single high number needs context, not panic or self-treatment.
Why uric acid levels rise
Uric acid rises when production and removal fall out of balance. In many adults, the kidneys are not clearing enough uric acid. This does not always mean kidney disease, but kidney function is an important part of the workup. If your high result appears with abnormal kidney tests, swelling, blood pressure changes, or urinary symptoms, a clinician may look more closely at kidney health. For broader kidney-related reading, the Nephrology Hub can help you navigate related topics.
Several factors can increase uric acid or make it harder to clear. These include family history, chronic kidney disease, dehydration, insulin resistance, higher body weight, rapid weight loss, heavy alcohol intake, and frequent intake of high-fructose drinks. Some medicines can also affect uric acid, including certain diuretics and low-dose aspirin. Do not stop a prescribed medicine on your own. Ask the prescriber whether the result changes your risk or follow-up plan.
Cell turnover can also raise uric acid. This may happen during some cancer treatments, with certain blood disorders, or during severe illness. These situations need medical supervision because uric acid can rise quickly and affect the kidneys.
Food matters, but food is not the only cause. High-purine foods can add to the uric acid load, especially when several triggers stack together. Still, blaming one meal often misses the bigger picture. Kidney clearance, genetics, alcohol, sugary drinks, and medication history may matter as much as diet, or more.
Symptoms: why high uric acid can be quiet
High uric acid often has no early symptoms. Many people first learn about it after routine blood work, a gout attack, or a kidney stone. This is why the phrase high uric acid symptoms can be misleading. The blood level itself is silent for many people; symptoms usually come from complications.
Gout symptoms often start suddenly. A joint may become intensely painful, swollen, warm, red, or hard to touch. The big toe is a classic site, but gout can affect ankles, knees, wrists, fingers, or elbows. Gout can resemble infection or other inflammatory joint conditions, so a hot swollen joint deserves careful review. The Rheumatology Hub offers related joint and inflammatory condition resources.
Kidney stone symptoms can feel different. A stone may cause sharp pain in the side, back, lower belly, or groin. Some people notice blood in the urine, nausea, vomiting, frequent urination, or pain while urinating. Fever, chills, inability to pass urine, or severe uncontrolled pain may signal an urgent problem.
Symptoms are not reliably different for women and men. However, lab reference ranges may differ, and risk patterns can change with age, menopause, kidney function, and medicines. During pregnancy, a high uric acid result should be interpreted by an obstetric clinician, especially if blood pressure is high or swelling is concerning.
Tests and numbers: making sense of serum uric acid
A uric acid blood test measures serum uric acid, usually reported in mg/dL. Your clinician may repeat the test because levels can fluctuate with hydration, recent meals, alcohol intake, illness, kidney function, and timing around a gout flare. A normal result during a painful joint attack does not always rule out gout, and a high result does not prove gout by itself.
The safest interpretation asks three questions. First, is the level truly high for the lab range and your health context? Second, are there symptoms such as gout attacks, kidney stones, or urinary problems? Third, are there underlying contributors that can be modified or treated?
Additional testing may include kidney function blood tests, urine testing, imaging for stones, or joint fluid testing if gout is uncertain. Joint fluid analysis can identify urate crystals, but not everyone needs this test. The right workup depends on symptoms, exam findings, and history.
People often ask about a safe uric acid range. There is no single safe number for every person. Many labs flag results above about 6 mg/dL in women or 7 mg/dL in men, while people treated for gout may have a lower target chosen by their clinician. A target used for gout management should not be applied to every person with one mildly high result.
Safer control starts with the cause, not just a food list
Hyperuricemia treatment depends on risk. Someone with one mildly elevated result and no symptoms may need repeat testing and risk review. Someone with repeated gout attacks, uric acid stones, kidney disease, or very high levels may need a more active plan. Your clinician may consider diet changes, medicine review, kidney evaluation, or urate-lowering therapy depending on the full picture.
Diet changes can support control, especially when they are realistic. A low purine diet for uric acid usually limits organ meats, some game meats, certain seafood, and heavy meat-based portions. Beer and liquor can raise risk for some people. Sugary drinks, especially those with high-fructose sweeteners, can also increase uric acid production. Water, balanced meals, and steady routines are more useful than crash diets.
Rather than memorizing a universal list of 10 foods that trigger uric acid, look for patterns. Common trigger groups include organ meats, large red meat portions, anchovies, sardines, mussels, scallops, some gravies, beer, liquor, and sweetened beverages. Individual response varies. Food logs can help, but they should not become restrictive or stressful.
Weight management may help some people, but rapid weight loss can temporarily raise uric acid. A gradual, sustainable plan is safer than fasting or extreme carbohydrate restriction. If you live with several chronic conditions, general lifestyle planning may feel easier when it focuses on patterns rather than perfection. BorderFreeHealth readers can also review Chronic Illness Lifestyle for broader diet and movement context.
Quick tip: Bring your medication list and recent lab results to appointments.
Blood pressure, kidney function, diabetes risk, and body weight can overlap with uric acid concerns. Some blood pressure medicines affect uric acid, while others may be more neutral for some patients. This does not mean a medicine is wrong for you. It means your prescriber should see the whole medication list before making changes. People balancing these issues may find Managing High Blood Pressure useful for related questions.
Where medicines fit into care
Medication decisions depend on symptoms, risk, and medical history. Urate-lowering medicines can reduce uric acid production or help the body remove more uric acid. They are often considered for people with recurrent gout, certain kidney stone patterns, or other higher-risk situations. They are not automatically prescribed for every person with asymptomatic hyperuricemia.
Gout flare treatment is a different issue from long-term uric acid control. Anti-inflammatory medicines may be used for acute flares when appropriate, while urate-lowering therapy aims to reduce future crystal formation. Starting, stopping, or changing these medicines can affect flare risk and safety. This is one reason medication decisions should be supervised.
Some people need extra caution. Kidney disease, liver disease, pregnancy, drug allergies, heart disease, and complex medication lists can change the safest option. If prescription medicine becomes part of your care, access also depends on eligibility, prescriber review, and local rules. BorderFreeHealth works with licensed Canadian pharmacy partners for eligible prescriptions.
Do not use supplements or over-the-counter products as a substitute for evaluation. Some products can interact with medicines or affect the kidneys. If you use herbal products, vitamins, or protein supplements, include them on your medication list.
Hyperuricemia, gout, and kidney stones: how they connect
Hyperuricemia and gout are closely linked, but they are not the same thing. High uric acid increases the chance that urate crystals can form. Gout happens when those crystals trigger inflammation in a joint or nearby tissue. Many people with high uric acid never have gout, while some people with gout may have a normal uric acid level during a flare.
Kidney stones are another possible complication. Uric acid stones can form when urine is too acidic and uric acid is concentrated. Not all kidney stones are uric acid stones, so stone analysis and urine testing may help guide prevention. Hydration, urine chemistry, diet, and underlying conditions all matter.
There is also ongoing research into links between high uric acid and metabolic or cardiovascular conditions. These links do not prove that uric acid is always the cause. Still, they remind clinicians to look beyond a single lab number. Older adults reviewing broader cardiovascular risk may also benefit from Heart Health After 60.
Questions to discuss with your clinician
A focused conversation can prevent both overreaction and delay. Ask what your number was, what range the lab uses, and whether repeat testing is needed. Ask whether kidney function, urine tests, or stone history changes the interpretation. If you have joint pain, ask whether gout, infection, injury, or another inflammatory condition needs consideration.
- Lab context: What was the uric acid level and reference range?
- Symptom pattern: Are joint or urinary symptoms present?
- Kidney review: Are creatinine, eGFR, or urine tests abnormal?
- Medicine check: Could any current drug affect uric acid?
- Food pattern: Are alcohol, sweet drinks, or high-purine foods frequent?
- Treatment threshold: Is monitoring enough, or is therapy being considered?
If you have sudden severe joint pain with fever, seek urgent care. The same applies to severe flank pain, vomiting, blood in urine, inability to urinate, or signs of dehydration. These symptoms need prompt assessment because infection, obstruction, or other serious conditions can overlap with uric acid problems.
Authoritative Sources
- NCBI Bookshelf reviews hyperuricemia definitions and causes.
- MedlinePlus explains uric acid blood and urine testing.
- The American College of Rheumatology summarizes gout management guidance.
Hyperuricemia is manageable for many people, but the safest path is personal. Treat the lab result as a signal to review symptoms, kidney health, medicines, food patterns, and long-term risk with a qualified professional.
This content is for informational purposes only and is not a substitute for professional medical advice.